
What is a colonoscopy?
Colonoscopies are one of the most important preventive examinations to maintain our (intestinal) health and detect tissue changes and bowel cancer – in time! Although the technical and scientific development of colonoscopy has made great progress, many people still shy away from the examination. Personal experience or digestive complaints reported by family and friends are often a reason not to have a colonoscopy. Similar to a colonoscopy, many people also choose to undergo colonic cleansing treatments to support their digestive tracts, however, the laxative solutions used in such a procedure also have an impact on our gut flora.
What are colonoscopies for?
The name of the procedure “colonoscopy” comes from “colon” (= the middle section of the large intestine) and “skopie” (= to look at, examine). The history of colonoscopy began in the 1960s, when a device was developed at the University of Tokyo to view the inside of the intestines.
During a colonoscopy, inflammation, polyps and tissue changes, including bowel cancer, can be detected and clarified at an early stage.
Around 50 years ago, the Swiss gastroenterologist Peter Deyhle developed a procedure to remove intestinal polyps during a colonoscopy. Today, this preventive examination is recommended to all around the age of 50 in order to examine the colon and the last centimetres of the small intestine from the inside.
Why is a colonoscopy recommended? Medication, ulta-processed food, stressful environmental influences, but also a genetic predisposition can lead to various digestive problems. During a colonoscopy, the doctor can not only examine the entire colon, but also remove tissue samples and perform minor surgical procedures.
Why are colonoscopies so important?
A colonoscopy can detect and clarify inflammation, polyps and tissue changes, including bowel cancer, at an early stage! Nevertheless, many people still shy away from this important preventive examination. This fear is unfounded, however, because colonoscopies are only ever performed by medical professionals with special training, usually a gastroenterologist. In general, a colonoscopy is a safe and painless procedure with a very low risk of complications – and is usually completed in less than half an hour. Alternatively, it is possible to examine the intestine with a capsule endoscopy (a small capsule with an integrated camera is swallowed) or to view it from the outside with a computer tomography (CT) or magnetic resonance imaging (MRI). However, these alternatives are more costly and/or time-consuming – and for taking a tissue sample or removing polyps and the like, a colonoscopy is performed anyway, so a colonoscopy is an efficient 2-in-1 examination!
How to prepare for a colonoscopy
In order to have a clear view in the intestine, it is necessary to empty it completely. On the one hand, this requires a short period of fasting, which, as you will learn later, can have a number of benefits: no food that is difficult to digest is allowed 24 hours before the procedure. The last solid meal is lunch one day before the colonoscopy. From then on, you should only drink broth, tea and water. Foods containing grains in particular should be avoided for a few days beforehand, as they tend to stick to the intestinal wall. In the case of general intestinal sluggishness, it may be advisable to start the short-term dietary change even earlier.
In addition, a thorough bowel cleanse is required. This is important because the bowel can only be reliably assessed when it is completely empty. For this purpose, a laxative, the so-called intestinal lavage, is used – and in addition to the technical advances, there have also been improvements here. “When I think back to the time 30 years ago, people had to come early in the morning or in the middle of the night and drink six litres of an aqueous solution. Today, that is limited to about two litres spread over two days. That is already considerably more pleasant,” explains intestinal specialist Prof. Dr. med. Joachim Labenz from the Diakonie Klinikum Jung-Stilling in Siegen.
The significant reduction of laxatives that one has to drink increased the likelihood of people making their appointments to have the procedure. “Personally, I feel that this is a clear step forward. In addition, we now have many more doctors who are very qualified and can draw on a lot of experience, which has greatly reduced the risk of complications.”
Of course, all the preparation is done in close consultation with the doctor in charge. Incidentally, the doctor should also be informed if the patient regularly takes medication, because the laxative may influence its effect. Some medications, e.g. those with blood-thinning agents, may have to be discontinued before the colonoscopy.
So if you weigh up the advantages and possible disadvantages of colonoscopy, the preparation is not a big challenge and certainly not an obstacle to a colonoscopy.
What happens during a colonoscopy?
A colonoscopy is usually completely painless. However, for many people it is more pleasant not to be consciously aware of the examination. It is advantageous for the doctor if the patient remains fairly still, as involuntary or sudden movements could lead to minor injuries. “That is why colonoscopy is now usually done with light sedation. This means that the examination itself is no longer unpleasant for the patient,” adds gastroenterologist Prof. Labenz, MD.
For a colonoscopy, the patient is placed in a comfortable lateral position, then the colonoscope, which resembles a thin, flexible tube, is inserted into the anus with the help of a lubricant. Air is blown into the bowel to help smooth out the folds of the bowel so that even the smallest changes can be seen more clearly. Here, many doctors, like Prof. Dr. med. Labenz, also use an advanced alternative. “Another development that makes the examination more comfortable for the patient is the use of CO2 instead of room air. The body breaks down CO2 much faster. That’s why people no longer have such a pronounced bloated belly after the examination, which many find very unpleasant. Thanks to the use of CO2, this can be reduced significantly.”
High-tech support for the all-in-one examination
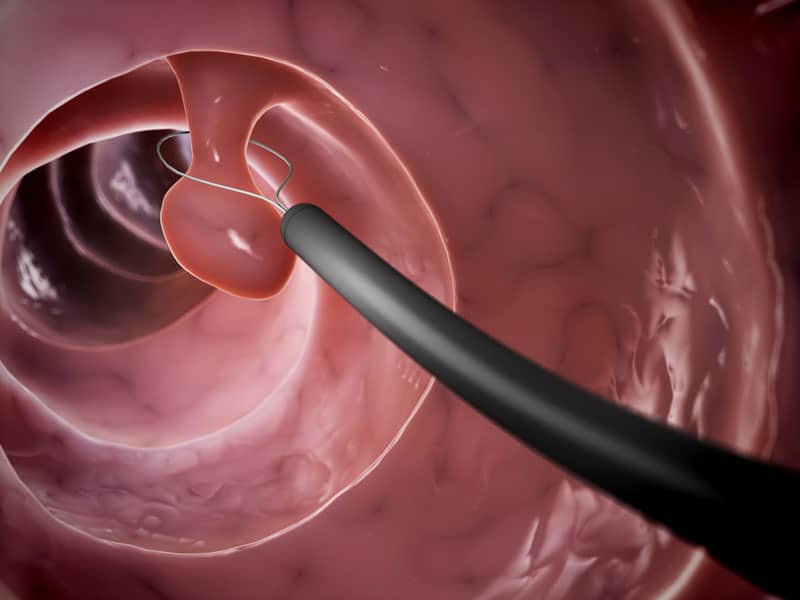
Then the colonoscope, which allows exposure and video transmission, is carefully guided through the entire colon. The doctor looks at everything on a monitor and examines the entire inner wall of the intestine. After the examination, the intestinal mucosa can be analysed in more detail using the recorded images. If there are any abnormalities on the intestinal wall, the doctor can immediately take samples with the help of tiny forceps and have them examined in the laboratory. In particular, the detection of so-called polyps is a central task of colonoscopy: these mucosal protrusions in the (large) intestine are harmless in themselves, but they can develop into bowel cancer. Therefore, timely removal is recommended.
“We have made great progress in the detection of polyps, on the one hand through improved technology and on the other hand through the increasing experience of the examination team. In the future, artificial intelligence could also be used. Machines and programmes that help the doctor detect very small polyps. This increases the number of polyps detected in time to be removed preventively. Even the minimal risk of post-operative bleeding when polyps are removed is not a problem, because the bleeding can be stopped quite easily.”
For this purpose, the colonoscope contains small loops via a channel that are passed around the polyps and separate them from the intestinal wall. This is also usually completely painless. The colonoscopy itself usually takes less than half an hour and is done on an outpatient basis. Inpatient treatment is only necessary in exceptional cases. Once the examination is complete, the tube is carefully removed again and it is immediately possible to eat and resume your usual daily life. It is only recommended to go home accompanied, because driving a vehicle (car, motorbike, bicycle) is not allowed due to the light sedation.
What does a colonoscopy have to do with the gut microbiome?
A colon cleanse temporarily leads to a significant change in the natural intestinal flora. Since science knows more about the central importance as well as the sensitivity of the human microbiome, laxatives are used more sparingly. Nevertheless, the gut flora is destroyed during the preparation for a colonoscopy. An important part of those bacteria that are responsible for our digestion and immune system is temporarily lost – digestion no longer functions properly and the absence of good bacteria allows germs to breed in the intestine. It can even take several weeks or months after a colonoscopy for the intestinal flora to recover. The change in the microbiome is noticeable in up to 80 % of patients after a colonoscopy. Almost half have bloating problems, followed by diarrhoea, abdominal pain and constipation – and these after-effects are precisely why many refuse to have another colonoscopy or do not have such an examination in the first place if family and friends tell them in detail about the side effects they have experienced.
Why is a colonoscopy important for your health?
The colonoscopy is not only the most important preventive examination for the intestine: the preparatory measures can also have a great health benefit for many people. There are places in the intestine, for example in diverticula (outward protrusions of the intestine, the opposite of polyps) or in the mouth of the appendix, where faeces can accumulate for weeks and even months, rotting and putting a strain on the intestine and the body. This digestive residue is also removed by the laxative. “According to my observations, it has always been the case, especially in patients with diverticula, that the preparation for the colonoscopy is often good for them. I have patients who voluntarily do this twice a year – without a colonoscopy. Afterwards, they report that they feel much better for weeks or even months,” the expert explains.
Probiotics – Colonoscopy recovery made easy
For Prof. Dr. med. Labenz, too, the connection between colonoscopy preparation, intestinal flora and intestinal complaints is of great relevance. That is why a clinical study was conducted: “It is quite clear that a colonoscopy affects the microbiome. And it seems to make sense to take a probiotic after a colonoscopy in order to increase the diversity, i.e. the quality of the intestinal microbiome.
We therefore studied whether the patients had complaints after a colonoscopy for four weeks and whether this was different either with a placebo or with the use of a probiotic. And we studied the composition of the intestinal flora with today’s modern methods to see if the probiotic had an effect on the diversity of the microbiome. It’s considered a quality characteristic of the microbiome: the more diverse it is, the healthier you are.”
The results of this study [1] are quite astounding. In the probiotics group, the so-called alpha diversity, i.e. the diversity of the microbiome in the intestine of the respective patient, was indeed significantly higher than in the placebo group. Also remarkable was the significantly increased occurrence of one of the bacterial strains contained in the probiotic.
If someone wants to do something good for themselves after a colonoscopy, they should take a special probiotic for four weeks, this will help the gut and microbiome.
What is particularly interesting for all those who have shied away from a colonoscopy until now because of the resulting digestive complaints: Taking the probiotic resulted in significantly fewer days with constipation. In addition, significantly fewer days with digestive complaints such as diarrhoea or flatulence were recorded.
Source:
[1] Labenz, J. et al. Ein Multispezies-Probiotikum zeigt einen positiven Effekt auf das intestinale Mikrobiom und reduziert Darmsymptome nach einer oralen Darmlavage zur Vorsorge-Koloskopie: randomisierte, doppelblinde, plazebokontrollierte Multicenterstudie (COLONIZE). Z Gastroenterol. 60(08): 643–643 (2022) DOI 10.1055/s-0042-1755100 (Available in German only – EN translation of study: A multispecies probiotic shows a positive effect on the intestinal microbiome and reduces intestinal symptoms after oral bowel lavage for screening colonoscopy: randomised, double-blind, placebo-controlled multicentre study)
Author:
Professor Dr. Joachim Labenz: Professor Dr. Joachim Labenz: Private practitioner for gastroenterology & hepatology at Diakonie Klinikum Jung-Stilling, Siegen (D), emeritus director of Medical Clinic I
Find out more about OMNi-BiOTiC® COLONIZE now













































